At 47, Suzanne Zekavat wanted nothing more than to stay active and keep up with her two young daughters. But severe arthritis in both knees had diminished her mobility to the point that just taking the stairs was excruciating.
“I had tried injections and everything else under the sun, but my doctors told me nothing else could be done because my joints were bone-on-bone,” says Zekavat, who lives in Moorestown. “I was sick and tired of being in pain all the time.”
So, like a growing number of young female patients, Zekavat elected to undergo joint replacement surgery. She opted to have one knee replaced in 2014, followed by the second late last year.
“It was a tough decision, because it’s elective surgery – you’re still going under anesthesia, and there are risks,” says Zekavat. “I wondered if I was doing the right thing, and I had a lot of anxiety – I didn’t know what to expect. But the pain was so bad on a day-to-day basis that I knew I needed to have it done.”
Now pain-free for the first time in years, Zekavat just finished up physical therapy and has returned to swimming, Pilates and even a weekly spinning class. “I am so happy I made the decision to have the surgery now, instead of putting it off until I was older,” she says. “I want to enjoy life while I’m still young, fit and active.”
Zekavat’s decision reflects a growing trend in South Jersey and beyond, says Gregory Klingenstein, MD, of Reconstructive Orthopedics. “On average, the median age of patients opting to undergo knee and hip replacement surgery in the United States goes down year by year. There’s no ‘right’ age for replacement surgery, but better diagnoses and treatments are making a difference for younger patients.”
A 2014 study by the American Academy of Orthpaedic Surgeons (AAOS) found the rate of knee replacements among patients ages 65 to 84 increased 188 percent over a 10-year period, and a 2015 study by the U.S. National Center for Health Statistics discovered that hip replacements in patients ages 45 to 54 jumped 205 percent in that same period of time.
The majority of these patients, like Zekavat, suffer from serious arthritis. “Women have a much greater rate of arthritis than men,” says Thomas O’Dowd, MD, of Advocare South Jersey Orthopedic Associates. “Nationally, approximately 60.8 percent of patients complaining of arthritis as a whole are women. Of those who say arthritis significantly affects their life, 63 percent are women.”
Biology also plays a large part, says O’Dowd. “A man who is 5-foot-10 and a women who is 5-foot-10 are going to have very different gaits and different pressure on their joints even though they’re the same height. Plus, a woman’s pelvis is wider than a man’s, which is another reason why women tend to suffer more knee pain. Hormone fluctuations in women can also increase joint pain. Overall, it makes sense that more women are electing to have joint replacement surgery.”
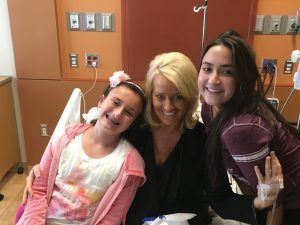
Suzanne Zekavat was alert and able to interact with her daughters shortly after knee replacement surgery
In other joint replacement cases, hip dysplasia is the culprit. “Hip dysplasia is much more common in women than men – the hip socket in women is very shallow from birth, and the cartilage wears out quickly,” says Klingenstein. “But another huge factor for the rise in both knee and joint replacement surgeries is obesity. Being obese places tremendous stress on the joints, and as the obesity epidemic gets worse and worse, we’re going to see a growing number of young patients who need joint replacement procedures.”
No matter the reason for the surgery, O’Dowd says, “younger women are usually less willing to be debilitated by joint pain. They want to be busy and active while they’re young. It used to be that people held off as long as possible, but it’s more accepted nowadays to have surgery while you’re young.”
While age is becoming less of a deciding factor in joint replacement surgery, O’Dowd says most doctors prefer to first try non-surgical techniques like physical therapy and steroid, cortisone or lubricant injections. “For patients who are overweight, one of the most successful ways to eliminate joint pain is weight loss,” he says. “But if you’ve exhausted all the options and you’re at the point that you’re taking anti-inflammatory medications like Motrin four times a day and still can’t be made reasonably comfortable, you have to do something.”
Thanks to new and improved technology, most replacement knee and hip joints are expected to last upwards of 20 years, according to the AAOS. There are hundreds of knee and hip replacement implant designs on the market, and a growing number of them are labeled as gender-specific. They claim to better mimic the size and shape of female bones, creating a more comfortable, custom-fitting implant with a wider range of motion.
No matter what type of implant your doctor uses, physical therapy is the key to getting back on your feet following surgery, says O’Dowd. “Most doctors get you up and walking shortly after surgery, and the following three to four weeks are the most important for recovery. The physical therapy process isn’t different for women or younger patients, but younger patients are more likely to be in better physical shape. This means they’re able to get back to their baseline function a little faster.”
And though minimally invasive procedures have become standard in joint replacement, it’s still major surgery, says O’Dowd. “It hurts. But the sooner you get moving, the better off you’ll be in the long run.”
Most patients, whether recovering from a knee or hip replacement, should aim to be walking without the assistance of a walker or cane within a few weeks. Hip replacement patients can expect a return to pre-surgery activity within three months, while knee replacement patients are usually back to normal activity within six to nine months.
In Zekavat’s case, she was able to ditch the walker and cane in just over a week. “I was very religious about doing physical therapy multiple times a week once I was out of the hospital, which I think made a huge difference,” she says. “I was pretty hard on myself and the pain was intense at first, but I was determined to get back to my life as soon as possible.”
“I was walking without limping very quickly and driving shortly thereafter. I think everyone around me was surprised at how quickly I was back in action,” she continues. “I would encourage any woman who is thinking about having the surgery to go for it now – don’t wait any longer.”














